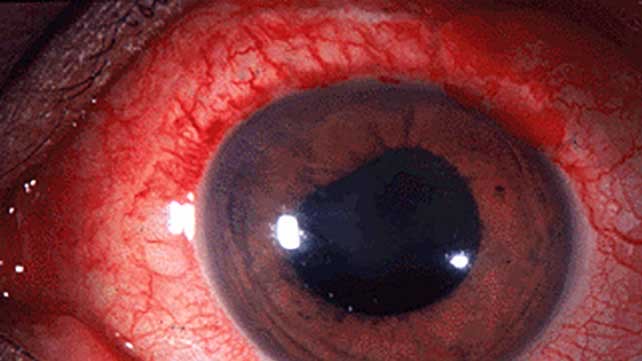
HAVE YOU HEARD ABOUT AN EYE CONDITION CALLED UVEITIS?
Uveitis is a form of eye inflammation. It affects the middle layer of tissue in the eye wall (uvea). Inflammation usually happens when your immune system is fighting an infection. Sometimes uveitis means your immune system is fighting an eye infection, but it can also happen when your immune system attacks healthy tissue in your eyes.
WHAT IS THE UVEA?
The uvea supplies blood to the retina. The retina is the light-sensitive part of the eye that focuses the images you see and sends them to the brain. It’s normally red due to its blood supply from the uvea.
The uvea is the middle layer of the eye between the sclera (white part of the eye) and the retina (light-sensitive layer at the back of the eye). It has 3 parts:
1 Iris (the colored part of the eye)
2 Ciliary body (the part of the eye that helps the lens focus)
3 Choroid (the part of the eye that connects the retina to the sclera)
Uveitis warning symptoms often come suddenly and get worse quickly. They include eye redness, pain and blurred vision. The condition can affect one or both eyes, and it can affect people of all ages, even children.
Possible causes of uveitis are infection, injury, or an autoimmune or inflammatory disease. Many times a cause cannot be identified.
Uveitis can be serious, leading to permanent vision loss. Early diagnosis and treatment are important to prevent complications and preserve your vision.
WHAT ARE THE SYMPTOMS OF UVEITIS?
The following symptoms may occur in one or both eyes:
1 Severe redness in the eye
2 Pain
3 Dark floating spots in your vision, called floaters
4 Light sensitivity
5 Blurred vision
Symptoms may occur suddenly and get worse quickly, though in some cases, they develop gradually. They may affect one or both eyes.
TYPES OF UVEITIS
The type of uveitis you have depends on which part or parts of the uvea that are inflamed:
- Anterior uveitis affects the inside of the front of your eye (between the cornea and the iris) and the ciliary body. It is also called iritis and is the most common type of uveitis.
- Intermediate uveitis affects the retina and blood vessels just behind the lens (pars plana) as well as the gel in the center of the eye (vitreous).
- Posterior uveitis affects a layer on the inside of the back of your eye, either the retina or the choroid.
- Panuveitis occurs when all layers of the uvea are inflamed, from the front to the back of your eye.
RISK FACTORS OF UVEITIS
People with changes in certain genes may be more likely to develop uveitis. Cigarette smoking has been associated with more difficulty to control uveitis.
WHAT CAUSES UVEITIS?
The cause of uveitis is often unknown and frequently occurs in otherwise healthy people. It can sometimes be associated with another illness such as an autoimmune disorder or an infection from a virus or bacteria.
- An autoimmune disease occurs when your immune system attacks a part of your body. Autoimmune conditions that may be associated with uveitis include:
1 rheumatoid arthritis
2 ankylosing spondylitis
3 psoriasis
4 arthritis
5 ulcerative colitis
6 Kawasaki disease
7 Crohn’s disease
8 sarcoidosis
- Infections are another cause of uveitis, including:
1 AIDS
2 herpes
3 CMV retinitis
4 West Nile virus
5 syphilis
6 toxoplasmosis
7 tuberculosis
8 histoplasmosis
- Other potential causes of uveitis include:
1 exposure to a toxin that penetrates the eye
2 bruising
3 injury
4 trauma
COMPLICATIONS
Left untreated uveitis can cause complications, including:
1 Retinal swelling (macular edema)
2 Retina scarring
3 Glaucoma
4 Cataracts
5 Optic nerve damage
6 Retinal detachment
7 Permanent vision loss
HOW IS UVEITIS TREATED?
Treatment for uveitis depends on the cause and the type of uveitis. Usually, it’s treated with eye drops. If uveitis is caused by another condition, treating that underlying condition may eliminate the uveitis. The goal of treatment is to reduce inflammation in the eye, as well as in other parts of the body, if present.
Visit your eye care practitioner once you notice sudden redness, pain and blurry vision, for proper eye examination and adequate treatment.